The Takeaway
Obstructive sleep apnea increases the risk of developing hypertension, heart disease including heart attacks and heart failure, stroke, and diabetes.
There is increasing evidence that untreated obstructive sleep apnea (OSA) can have a significant impact on your personal health. Successful treatment of OSA may reduce the risks of these related ailments.

Why does OSA increase the risk of having other health problems?
Studies suggest that having OSA raises the heart rate and increases blood pressure, placing stress on the heart. This may be because apneas frequently reduce blood oxygen levels, activating the branch of the nervous system responsible for increasing heart performance. In addition, levels of chemicals in the blood that cause inflammation and promote elevations in blood sugar rise. Such inflammation can damage the heart and blood vessels. 1, 2 Both hypertension and diabetes increase the risk for heart disease, and the likelihood of being diagnosed with one of these illnesses increases as a result of OSA.
Hypertension
High blood pressure is a common chronic medical condition. It afflicts over 40% of people between the ages of 50 and 60 years of age in the United States. OSA is a risk factor for the development of hypertension.3 Approximately 50% of those with sleep apnea have hypertension. In fact, elevated blood pressure might be the only clue that a person has OSA. Fortunately, treatment of OSA may result in better control or even resolution of hypertension.
Heart Disease
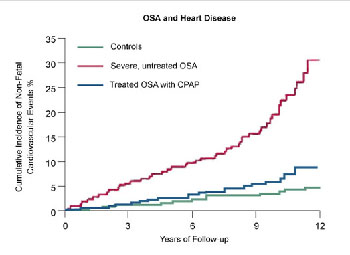
Coronary artery disease occurs in 67% of the adult population of the United States. It frequently results in heart attacks and premature death. Evidence indicates that OSA might be a risk factor for future heart attacks or angina pectoris (chest pain related to blockage of blood vessels supplying the heart), and middle-aged men might be at particular risk (see Figure 3).4
Dr. Stuart Quan explains the serious consequences
of untreated obstructive sleep apnea.
Stroke
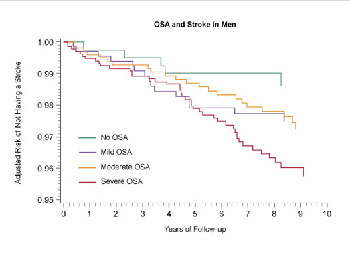
Having a stroke can be a devastating event, with the potential for severe disability or death. OSA might be a risk factor for having a stroke (see Figure 4), and recovery after a stroke might be delayed in people with OSA.5 Conversely, people who have had a stroke are more at risk of developing OSA.
Diabetes Mellitus
Coinciding with the increase in obesity in the United States, more and more people are developing type 2 diabetes. Research indicates that blood sugar (glucose) levels are higher among people with OSA. However, it appears that treatment of OSA may improve blood sugar levels.
Premature Death
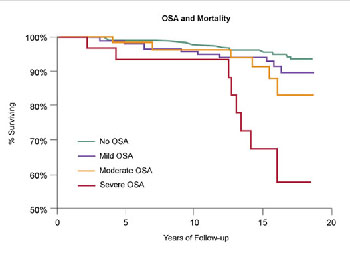
Because OSA is associated with a number of chronic medical conditions, not surprisingly, several studies have shown an association between OSA and increased likelihood of premature death (see Figure 5).6 Middle-aged men appear to be at greatest risk, with the cause of death most commonly related to cardiovascular disease. Football star Reggie White, a Hall of Fame defensive end for three NFL teams, died of cardiac and pulmonary problems that were likely intensified by his sleep apnea. He was 43.
Dr. Susan Redline describes how each apnea can increase the risk of cardiovascular problems.
References
1. Budhiraja R, Parthasarathy S, Quan SF. Endothelial dysfunction in obstructive sleep apnea. J Clin Sleep Med 2007;3:409-15.
2. Dempsey JA, Veasey SC, Morgan BJ, O'Donnell CP. Pathophysiology of sleep apnea. Physiol Rev 2010;90:47-112.
3. Budhiraja R, Sharief I, Quan SF. Sleep disordered breathing and hypertension. J Clin Sleep Med 2005;1:401-4.
4. Marin JM, Carrizo SJ, Vicente E, Agusti AG. Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet 2005;365(9464):1046-53.
5. Redline S, Yenokyan G, Gottlieb DJ, et al. Obstructive sleep apnea-hypopnea and incident stroke: the sleep heart health study. Am J Respir Crit Care Med 2010;182:269-77.
6. Young T, Finn L, Peppard PE, Szklo-Coxe M, Austin D, Nieto FJ, Stubbs R, Hla KM. Sleep disordered breathing and mortality: eighteen-year follow-up of the Wisconsin sleep cohort. Sleep. 2008 Aug;31(8):1071-8.