The Takeaway
- Positive airway pressure (PAP) therapy is the best and most common treatment for obstructive sleep apnea.
- Choose the PAP mask that is most comfortable for you.
- Common problems with PAP therapy all have solutions
As described in Nonsurgical Treatments, positive airway pressure (PAP) treatment involves placing a small mask or nose tubes (also known as "nasal pillows") over the nose or nose and mouth and blowing compressed air into the lungs. This is the most common form of treatment for obstructive sleep apnea (OSA), and it is useful to understand the testing, appliances, and challenges inherent to using PAP.
Testing for PAP
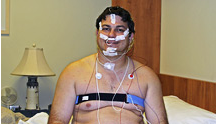
If a sleep study has shown that you have apnea, you may get a prescription for a PAP device. However, before a PAP prescription can be written, sometimes additional testing is performed to determine the level of air pressure needed to resolve the apnea and the type of device that will deliver it.
This additional testing is done again with polysomnography. During this polysomnography, the patient uses PAP therapy. Through this test, the level of PAP that resolves the apneas and hypopneas is determined. Often, this is called a "titration study."
In many cases, the diagnosis of OSA and titration for PAP are done in a single night; this is called a "split night" study. In "split night" studies, the first few hours of the polysomnography confirm the diagnosis of moderate to severe OSA. After confirmation, the rest of the night is used to titrate PAP.
As an alternative to a PAP titration, in many cases the correct level of PAP is determined using an automatically adjusting PAP device (AutoPAP). Either at home or in the sleep laboratory, the AutoPAP is worn, and the device adjusts the pressure to the level that eliminates the apneas and/or hypopneas. This pressure then can be used to set the level of CPAP. In some patients, AutoPAP is continued as ongoing treatment. However, use of AutoPAP is not appropriate for all cases, and its use should be decided by a sleep specialist.
Monitoring PAP Therapy
Most current PAP devices have the capability of monitoring usage and effectiveness. This is done by either a modem or a SCD card incorporated into the device. If a modem is used, data is transmitted into the cloud where it can be retrieved using a computer or a mobile device. If an SCD card is employed, the data is recorded onto the card where it can be downloaded manually onto a local computer. In both cases, the device provides information on a continuous basis on usage, pressures patterns, leaks from the PAP mask, and the amount of OSA that is still present while using PAP. This information helps the patient's sleep specialist or clinician determine whether PAP is effective and can assist in resolving challenges to PAP use. In addition, many PAP devices can be used in conjunction with an "app" so that the patient can self-monitor usage and effectiveness by using their own mobile device or computer.
Types of PAP Devices
- CPAP: Continuous Positive Airway Pressure is the most commonly used PAP device. With CPAP, the level of pressure delivered to the airway is the same during both inhalation and exhalation.
- Bilevel PAP (BPAP): With Bilevel PAP, the pressure during inhalation is higher than during exhalation. The pressures needed to control apnea and hypopnea events with Bilevel PAP are sometimes lower than with CPAP. Because some persons have difficulty tolerating high CPAP pressures, Bilevel PAP may be used when pressures required for CPAP are relatively high. Some BPAP devices have the capability to automatically adjust the inhalation and exhalation pressures in order to better control apneas and hypopneas.
- AutoPAP (APAP): Auto-adjusting PAP devices automatically vary PAP pressures during the night to the lowest levels required to eliminate apneas and hypopneas. Some persons with OSA may find AutoPAP devices more comfortable to use. Most devices can easily be switched between CPAP and APAP.
- Adaptive Servo Ventilation (ASV): With ASV, the device continuously monitors breathing pattern breath by breath. As the amount of air on each breath increases or decreases, the device appropriately adjusts its delivered air pressure to maintain a constant breath volume. It is not generally used for most persons with OSA, but can be helpful in the treatment of patients with both OSA and central sleep apnea.

Additional Features
For the basic function of applying pressure to the airway, there is generally little difference among PAP devices. However, they do vary in shape, size, weight, and additional features. Commonly found features include the following:
- Ramping: This feature allows the PAP device on start-up to gradually increase the pressure over a short period of time until the prescribed pressure is reached. Some users find that this allows them to fall asleep more easily and improves their ability to wear PAP.
- Pressure Relief: With pressure relief, at the beginning of exhalation, a small decrease in pressure occurs. The amount of pressure reduction is adjustable. Some users find that this makes use of PAP more tolerable by making it easier to exhale.
- Humidification: With PAP, large amounts of air move in and out of the nose, mouth, and upper airway. This can lead to drying of the air passages. Most PAP machines incorporate or permit the addition of humidifiers to add moisture to the air that is breathed in. This is especially important in dry, arid climates. Heated humidifiers add more moisture than humidifiers that do not heat the inhaled air.
Types of PAP Masks

There are many styles of PAP masks. The most important distinction is between those that deliver air via the nose, and those that deliver air via the nose and mouth. The latter are generally reserved for people who are mouth breathers during sleep. A comfortable, well-fitting mask with no more than minimal air leak is essential. There are no differences in efficacy among the large number of mask types. The best mask is the one you find comfortable and will wear regularly.
Common Challenges with PAP Use
Although there can be challenges to using PAP therapy, many can be overcome by working with an experienced healthcare practitioner. Approximately two-thirds of people who are prescribed PAP therapy find that it is a good long-term solution to their OSA. Some problems with PAP, and proposed solutions, are as follows:
- Nasal stuffiness or congestion: Possible solutions: greater humidification, prescription nasal sprays
- Leaks around the mask: Possible solutions: alternative mask or headgear
- Excessive noise: Possible solutions: check machine for a mechanical problem, cover machine to muffle noise
- Redness or irritation where the mask or mask straps touch the skin: Possible solutions: alternative mask or headgear, padding where irritation occurs
- Claustrophobia: Possible solution: gradual habituation program
- Too much pressure: Possible solutions: temporary drop in pressure, AutoPAP, Bilevel PAP, pressure relief, ramping (the gradual increase in pressure on start-up, see above).
- Dry mouth: Possible solutions: full-face mask, greater humidification
- Excess Water in the Tubing: Possible solutions: insulating the tubing, decreasing the humidification setting, and/or using tubing that can be temperature adjusted.
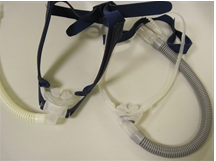
Dr. Geoffrey S. Gilmartin explains that a poorly fitting mask can make CPAP treatment difficult.